|
|
|
Breast/Ovarian Cancer: Woman at High Risk
Patient Identification
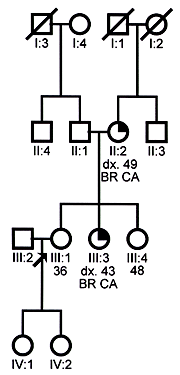
- Jane (denoted by arrow on pedigree) is a 36-year-old white non-Jewish woman who came in because she was concerned about her risk for developing breast cancer.
Relevant Past Medical History
- Due to her high anxiety regarding cancer, Jane has had 5 previous mammograms and has been receiving annual clinical breast exams (CBE).
- She performs weekly breast self-exams (BSE).
- She is overweight but has been exercising, resulting in a loss of 30 pounds.
- She has had problems with her menstrual cycle and is on oral contraceptives.
- She recently became a vegetarian and has stopped drinking alcoholic beverages.
Family History
- Jane's mother (II:2) was diagnosed with unilateral breast cancer at age 49. She underwent a mastectomy followed by chemotherapy and is alive and well.
- Jane's sister (III:3) was recently diagnosed with unilateral breast cancer at age 43. She underwent a lumpectomy and is currently receiving chemotherapy.
Counseling and Risk Assessment Session
- Jane believed that her chance of developing breast cancer was very high, greater than 75%.
- Based on the Claus model, her cumulative risk for developing breast cancer to age 79 is about 35%. The Claus model was used instead of the Gail model because Jane has a family history of breast cancer. Limitations of the model were presented.
- Based on the Couch model, the probability of Jane's mother or sister carrying a BRCA1 gene mutation is about 5% (CI=2.3-10.8%). Because Jane had a 50/50 chance of inheriting a mutation from her mother, Jane's risk of carrying a BRCA1 mutation is about 2.5%, half that of her mother. As the model only predicts the probability of a BRCA1 mutation, the number is doubled to obtain an estimate of the probability of carrying either BRCA1 or BRCA2 mutation. Therefore, Jane has about a 5% chance of having either mutation. Limitations of the model were presented.
- If Jane does carry a BRCA1/2 mutation, then her lifetime risk for developing breast cancer is 50-85%, compared to about 12% for the general population. Her lifetime risk for ovarian cancer also increases to 15-45%, compared to the 2% risk for the general population.
Recommendations
- Jane is in a high risk group.
- Increase CBE by a qualified health care provider to 2-3 times per year.
- Perform monthly BSE. During the visit, a nurse practitioner taught Jane how to perform a thorough BSE.
- Continue annual mammograms. Although the efficacy of mammography for this age group is not known, mammography was recommended because of the history of early onset breast cancer in the family.
- Continue regimen of exercise, low-fat diet, and abstinence from alcohol.
- Tamoxifen, found to decrease the incidence of breast cancer in high-risk women by 49%, was mentioned as a possible preventive option.
- Raloxifene was mentioned as a drug that is currently being studied in a clinical trial for its efficacy in preventing breast cancer. She is, however, premenopausal and thus not currently eligible.
- Jane raised the issue of prophylactic mastectomy as an option, especially if she were found to be gene positive.
- Her use of oral contraceptives was discussed in relation to breast cancer risk.
- Return to clinic in 6 months for CBE and further discussion.
Decision-Making Regarding Genetic Testing
- As Jane is very concerned about her risk for developing breast cancer, she is considering genetic testing. Initially, it would be appropriate to test living affected family members, either Jane's mother or sister, in this case. Because Jane is not Ashkenazi Jewish, for whom specific tests have been developed, a full sequencing of her BRCA gene must be performed.
- If her mother or sister tests negative for a BRCA mutation, then there is no need for further gene testing. Since BRCA1/2 mutations only explain 50-60% of inherited cancer family syndromes, Jane's family history may be due to other inherited factors.
- If her mother or sister tests positive, then Jane could be tested to see if she inherited the mutation. Jane has a 50/50 chance of having inherited the mutation. - Jane is concerned whether her sister, who was recently diagnosed, could deal with getting gene testing now so she will approach her mother.
- If her mother chooses to have a gene test, then Jane will then decide whether to have a gene test herself based on her mother's test result.
- Jane is concerned with the cost of testing but indicated that she would not let it be the only factor in her decision.
- Jane was informed of the possible insurance implications of genetic testing and she indicated that she would give them some consideration.
- Jane indicated that she would consider prophylactic mastectomy if she tests positive.
- Jane is concerned about having passed down the gene mutation to her two daughters.
References
- Easton DF; Bishop DT; Ford D; Crockford GP. Genetic linkage analysis in familial breast and ovarian cancer: results from 214 families. Am J Hum Genet 1993 Apr;52(4):678-701.
- Ford D; Easton DF; Bishop DT; Narod SA; Goldgar DE. Risks of cancer in BRCA1-mutation carriers. Lancet 1994 Mar 19;343(8899):692-5.
- Struewing JP; Hartge P; Wacholder S; Baker SM; Berlin M; McAdams M; Timmerman MM; Brody LC; Tucker MA. The risk of cancer associated with specific mutations of BRCA1 and BRCA2 among Ashkenazi Jews. N Engl J Med. 1997 May 15;336(20):1401-8.
- Ford D; Easton DF; Bishop DT; Narod SA; Goldgar DE. Risks of cancer in BRCA1-mutation carriers. Lancet 1994 Mar 19;343(8899):692-5.
Additional Resources
- NCI Cancer Genetics Information
- Breast Cancer Prevention Study Results
- Study of Tamoxifen and Raloxifene
- Breast Cancer Prevention Study Results
Feedback
- Please complete a brief evaluation of this case study.
- Submit a case for review.
Return to Case Study Main Page.
| © 2001-2 Mid-Atlantic Cancer Genetics Network modifed 9/3/04 | Privacy Statement | Questions/Comments bmay@jhmi.edu |

